 “Getting regular checkups is the best way to monitor your baby’s health as well as your own.Jupiterimages/Thinkstock
“Getting regular checkups is the best way to monitor your baby’s health as well as your own.Jupiterimages/Thinkstock
Congratulations, you’re pregnant! Now it’s time to be poked, prodded, monitored, measured and observed for about 40 weeks.
The amount of medical testing that happens to a mother between conception and delivery can seem overwhelming — but there are two lives at stake during this time, and it’s vitally important to make sure they both remain healthy. By taking the right tests at the right times, you will be ensuring the best possible chance of that happening.
This handy guide to the top 10 most important medical tests during pregnancy will help take some of the stress out of all of those doctor visits and let you get back to what truly matters — enjoying the anticipation of bringing a new life into your family.
Contents
- Complete Blood Count
- Sexually Transmitted Diseases
- Rh Factor Test
- Urine Tests
- Blood Pressure
- Fetal Ultrasound
- Multiple Marker Screening
- Glucose Tolerance Test
- Group B streptococcus
- Fetal Heart Rate Monitoring
10: Complete Blood Count
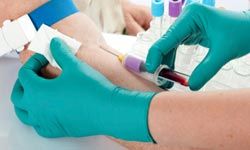 “Squeamish about having your blood drawn? Relax, if you can. It will make the whole process easier.iStockphoto/Thinkstock
“Squeamish about having your blood drawn? Relax, if you can. It will make the whole process easier.iStockphoto/Thinkstock
One of the first tests you’ll need when you become pregnant is a complete blood count or CBC. This measures a variety of factors in your blood, such as the number of white and red blood cells that you have. When you are pregnant, there are three important indicators your doctor will look for in your CBC test results: hemoglobin, hematacrit and your platelet count.
Hemoglobin is a protein in the blood that delivers oxygen to your cells, and hematacrit is a measure of red blood cells in the body. If either of these counts are low, it may indicate anemia, and your doctor would recommend a course of treatment to address the condition.
The platelets in your body are the substances that help your blood clot. It is critical that the platelet count be in the normal range because a woman looses a half liter of blood on average during pregnancy, and the platelets see to it that you don’t lose any more than that [source: Family Education]. If your count is unusually low, your doctor will conduct further tests to source the problem and administer treatment as appropriate.
9: Sexually Transmitted Diseases
In addition to checking the cellular composition of the blood during the early stages of a pregnancy, doctors will also screen blood samples for sexually transmitted diseases (STDs) such as HIV/AIDS, syphilis, herpes and hepatitis B and C. Additionally, a cervical swabbing will be used to check for gonorrhea and chlamydia.
Discovering these diseases early on in a pregnancy is vital, as they can all be passed on to the fetus. Syphilis and HIV can infect the baby while it is still in the womb, while other diseases like chlamydia, gonorrhea, hepatitis B and genital herpes can infect the baby during birth as it moves through the birth canal.
STDs can cause a range of complications for a baby including transmission of the disease itself, early delivery, eye infections (from gonorrhea and chlamydia), or much more severe consequences such as miscarriage or stillbirth (from syphilis).
In the case of HIV, medication can be given that reduces the risk of transmitting the disease to the baby from 25 percent to approximately 7 percent. Genital herpes, another viral infection, can’t be cured, but doctors might recommend a C-section if a woman has an outbreak at the time of delivery. In the case of hepatitis B, if the virus was contracted early in the pregnancy, there is a less than 10 percent chance the disease will be transmitted to the baby. If it was contracted later in the pregnancy, the transmission rate increases to approximately 90 percent [source: ACOG].
Chlamydia, syphilis and gonorrhea can be cured with baby-safe antibiotics.
8: Rh Factor Test
 “It’s possible that both expecting parents will need to undergo the Rh Factor Test.©iStockphoto/Thinkstock
“It’s possible that both expecting parents will need to undergo the Rh Factor Test.©iStockphoto/Thinkstock
Yet another test that’s conducted on a pregnant woman’s blood (and sometimes the father’s blood, too) early in the pregnancy, the Rh (or Rhesus) factor test looks for a type of protein found on the surface of the red blood cells. If you have the protein — as does approximately 85 percent of the population — you’re considered Rh positive and there is no potential issue [source: kidshealth.org]. If however, you lack the protein (Rh negative) and the father has it, complications can occur.
This is because the baby can inherit Rh-positive blood from the father. If this happens and then a baby’s blood mixes with the mother’s, the mother’s body could treat the baby like something to which it is allergic, and the immune system could attack the baby’s blood, causing a condition in the child known as hemolytic anemia.
It is rare for the blood of the fetus to mingle with the mother’s blood during gestation however, so this condition is often a concern for second pregnancies. That’s because intermingling of blood can occur during the first delivery and the next time an Rh-negative mother gets pregnant with an Rh-positive child, her antibodies will attack the fetus. This can be prevented by a simple vaccination around the 28th week of the pregnancy and again 72 hours after delivery of the first child.
7: Urine Tests
Pregnant women tend to need to urinate more than before they were pregnant. This isn’t such a bad thing when it comes to medical testing, because your urine is likely to be sampled several times during your pregnancy.
A urine test looks for certain markers in the fluid that can tell a doctor a great deal about the mother’s health. Chief among these is the amount of sugar in the blood. If it is too high it could indicate gestational diabetes, a condition that usually starts about halfway through the pregnancy. It is caused when pregnancy hormones stop insulin from removing sugars from the blood and can be corrected through diet and/or medication.
Your doctor will also be looking for protein in the urine, which could indicate a kidney infection; bacteria, which would point to a urinary tract infection; and ketones which occur when the body uses fats instead of carbohydrates for energy and could mean you are dehydrated or undernourished.
Optional Tests
Some tests, like those conducted through blood and urine analysis, are absolutely essential to both the baby and the mother’s health. Other tests, like Chorionic villus sampling (CVS), are usually optional. During a CVS test, which is usually done between the 10th and 12th weeks of pregnancy, a small group of cells is gathered from the placenta and analyzed for markers of conditions like Down Syndrome, Tay-Sachs disease, sickle-cell anemia and cystic fibrosis. The test is viable for women over 35 or anyone with a history of chromosomal abnormalities but there is a risk: approximately 1 in 100 women will miscarry as a result of the procedure [source: Mayo Clinic].
6: Blood Pressure
 “An expectant mother’s blood pressure is closely monitored throughout her pregnancy.Comstock/Thinkstock
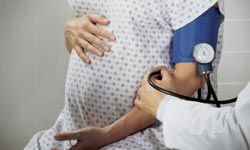
“An expectant mother’s blood pressure is closely monitored throughout her pregnancy.Comstock/Thinkstock
In addition to checking for the conditions previously described, your doctor will also be looking for signs of a condition known as preeclampsia in your blood and urine. In the blood, this could be expressed by a low platelet count and in the urine, the presence of protein might indicate that the condition is present.
Preeclampsia affects 7 percent of all pregnant women, especially first-time mothers and those carrying multiple children [source: Bissinger]. It is a rising of the blood pressure due to the pregnancy and typically happens late term. It can have serious health risks for both mother and child, such as a lack of blood flow to the placenta or placental abruption (the pre-delivery separation of the placenta from the uterus). If it is left untreated, it can advance to eclampsia, in which the mother can experience life-threatening grand mal seizures.
This is why it is critical to closely monitor blood pressure throughout the pregnancy — especially during the second half. But it’s also important to realize that high-blood pressure alone does not mean preeclampsia is occurring. It must be verified with protein in the urine, as well.
5: Fetal Ultrasound
This is perhaps the one test during a pregnancy that both father and mother look forward to, because it gives them their first glimpse of their new child. In an ultrasound test, a lubricating jelly is applied to a woman’s abdominal area and an ultrasound "wand" is guided across the surface of the skin. High-frequency sound waves are transmitted into the uterus and bounce back to return an image of the fetus.
Although parents will remember the test as the first time they got to see their baby’s heartbeat or find out the child’s sex, doctors conduct fetal ultrasounds for other reasons as well. The test is useful for discovering the gestational age of the baby which helps plan pre-natal care and predict a delivery date. It also helps locate the fetus and make sure that it is properly situated in the uterus, not in the fallopian tubes, which would indicate a dangerous condition known as an ectopic pregnancy. Fetal ultrasounds additionally make sure the baby is growing correctly and help identify any fetal abnormalities, examine the placenta to make sure it is healthy, and let expecting parents know if they’re only having one child or multiple births.
Fetal ultrasounds are typically conducted in the first trimester of the pregnancy and then again about midway through, but they can be used more than that if need be, as they are a very safe testing mechanism.
A Better View
During a standard ultrasound, the images that appear on the monitor or the printout parents are often given to take home can look more like abstract art than an actual rendering of a growing baby. 3-D ultrasounds are changing that dramatically. In these tests — which are becoming available around the country at a rapid pace — sound waves are returned to the sonogram’s wand from a variety of angles, instead of just bouncing straight back. This creates a much more accurate view of a fetus with depth to its physical features and makes the image recognizable, even by someone without special training.
4: Multiple Marker Screening
Multiple marker screening comes in two varieties: the triple screen test and the quad screen test. As you might imagine, the triple screen test looks for three substances in the blood produced by the fetus and/or placenta: alpha-fetoprotein (AFP), human chorionic gonadotropin (hCG) and estriol. The quad screen adds the substance inhibin A (Inh-A) to the mix.
By evaluating these substances in the blood at approximately the 15th to 20th week of pregnancy — and combining them with factors such as the mother’s age, weight and ethnicity — doctors are looking for signs of either neural tube defects like anencephaly or spina bifida, or for markers that might indicated Down syndrome.
The tests are about 80 percent accurate in predicting neural tube defects. The triple screen is approximately 60 percent accurate in spotting Down syndrome; the quad screen correctly identifies the condition 75 percent of the time [source: Bell]. Because of these relatively low percentages, and the fact that the tests tend to deliver high false-positives, if a doctor spots something amiss, she will likely recommend further testing such as an amniocentesis (see sidebar) or a sonogram (if you haven’t had one already). Sometimes, abnormal results from these tests can be explained by the fact that the pregnancy is actually further along then previously thought, which a sonogram would discover.
Amniocentesis
If a multiple marker screen test shows the possibility of problems with the fetus, a doctor might recommend an amniocentesis. In this procedure, a needle is inserted into the amniotic sac surrounding the fetus and a small amount of liquid is removed for analysis. There is, however, a risk to the test. Between one in 300 to one in 500 women will miscarry when the test is done in the second trimester. The risk is slightly higher when done earlier in the pregnancy [source: Mayo Clinic].
3: Glucose Tolerance Test
Around the 24th to 28th week of pregnancy, your doctor will likely recommend a glucose challenge test (GCT) to see if you might be developing gestational diabetes, a temporary condition in which insulin fails to break down enough glucose in the blood. The condition affects 2 to 5 percent of all pregnant women. If this test comes back positive, there is an approximately 30 percent chance that you have developed the condition and your doctor would conduct a glucose tolerance test (GTT) [source: Babycenter].
In this test, you are asked to drink a high-sugar liquid and then your blood is collected an hour later so that its sugar level can be measured. In about 15 to 23 percent of women, the blood sugar levels are indeed too high and a follow up three-hour GTT is scheduled, which typically rules out the condition [source: Babycenter].
If you do develop gestational diabetes, your doctor will work with you to develop a diet, exercise and possible insulin-supplementation plan. The condition nearly always ends after the baby is born.
2: Group B streptococcus
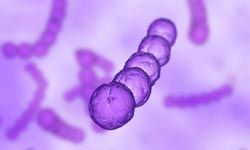 “Streptococcus bacteria looks innocuous, but it can cause serious birth defects.iStockphoto/Thinkstock
“Streptococcus bacteria looks innocuous, but it can cause serious birth defects.iStockphoto/Thinkstock
Although it only affects approximately one in every 2,000 babies born in the U.S., the bacterial infection known as group B streptococcus (GBS) can have serious consequences, so doctors (and the CDC) recommend that all pregnant women be tested — usually during the 35th to 37th week of their term [source: American Pregnancy Association]. The test is conducted through a vaginal and anal swab that checks for the bacteria, which is actually present in approximately 25 percent of all healthy women [source: American Pregnancy Association].
If the test comes back positive, there is a one in 200 chance that a baby will contract the disease during birth, which can lead to serious conditions like sepsis, pneumonia and meningitis. However, if antibiotics are administered intravenously during delivery, that risk drops to one in 4000 (source: American Pregnancy Association). Antiobiotics are particularly recommended for a woman whose water breaks more than 18 hours before delivery, who has a fever during labor, who goes into labor early, or who has a history of giving birth to a child who contracted the disease.
1: Fetal Heart Rate Monitoring
During labor, your doctor will likely monitor the heart rate of your baby. Due to contractions, which temporarily limit the flow of oxygen to the fetus, the baby’s heart rate will naturally change during birth. However, any changes that fall outside the normal range — approximately 110 to 160 beats per minute — could indicate that the baby is not getting enough oxygen overall, and steps would be taken to correct this [source: Lucile Packard Children’s Hospital at Stanford].
For EFM, two belts are wrapped around the mother’s abdomen — one which measures the baby’s heart rate and the other that measures contractions. Alternatively, internal monitoring may take place where an electrode is placed on the baby at the part nearest the cervix, which is usually the top of the head. For this type of monitoring, it is necessary for a woman’s water to have broken.
Lots More Information
Related Articles
- How Pregnancy Works
- 10 Diet Tips For Pregnant Women
- Fact or Fiction: Pregnancy
- Exercise During Pregnancy
- How To Prepare for Childbirth
Sources
- American College of Obstetricians and Gynecologists. "Fetal Heart Rate Monitoring During Labor." July 2011. (Aug. 9, 2011) http://www.acog.org/publications/patient_education/bp015.cfm
- American College of Obstetricians and Gynecologists. "Hepatitis B Virus in Pregnancy." 2008. (Aug. 9, 2011) http://www.acog.org/publications/patient_education/bp093.cfm
- American Pregnancy Association. "Group B Strep Infection: GBS." March, 2011. (Aug. 9, 2011) http://www.americanpregnancy.org/pregnancycomplications/groupbstrepinfection.html
- American Pregnancy Association. "Rh Factor." Apr. 2006. (Aug. 9, 2011) http://www.americanpregnancy.org/pregnancycomplications/rhfactor.html
- American Pregnancy Association. "Triple Screen Test." Feb. 2006. (Aug. 9, 2011) http://www.americanpregnancy.org/prenataltesting/tripletest.html
- babycenter.com. "Glucose screening and glucose tolerance tests." (Aug. 9, 2011) http://www.babycenter.com/0_glucose-screening-and-glucose-tolerance-tests_1483.bc
- Bell, Alison. "Testing: Trimester by Trimester: Your guide to prenatal tests." Parenting. (Aug. 9, 2011) http://www.parenting.com/article/testing-trimester-by-trimester?page=0,0
- birth.com.au. "Tests during pregnancy – what to expect and list." (Aug. 9, 2011) http://www.birth.com.au/Tests-offered-during-pregnancy/Tests-during-pregnancy-what-to-expect-and-list
- Bissinger, Craig L. "Preeclampsia: A Closer Look." pregnancy.org. (Aug. 9, 2011) http://www.pregnancy.org/article/preeclampsia-closer-look
- Family Education. "Test Performed During Pregnancy." (Aug. 9, 2011) http://pregnancy.familyeducation.com/prenatal-health-and-nutrition/tests-and-appointments/36317.html
- KidsHealth.org. "Rh Incompatibility." (Aug. 9, 2011) http://kidshealth.org/parent/pregnancy_center/your_pregnancy/rh.html#
- Lucile Packard Children’s Hospital at Stanford. "Common Tests During Pregnancy." (Aug. 9, 2011) http://www.lpch.org/DiseaseHealthInfo/HealthLibrary/pregnant/tests.html
- Maryland Department of Health and Mental Hygiene. "Multiple Marker Screening – A Prenatal Blood Test." (Aug. 9, 2011) http://fha.maryland.gov/genetics/muilti_marker.cfm
- Mayo Clinic. "Amniocentesis." (Aug. 9, 2011) http://www.mayoclinic.com/health/amniocentesis/MY00155/DSECTION=risks
- Mayo Clinic. "Chorionic villus sampling." (Aug. 9, 2011) http://www.mayoclinic.com/health/chorionic-villus-sampling/MY00154
- Mayo Clinic. "Fetal Ultrasound." (Aug. 9, 2011) http://www.mayoclinic.com/health/fetal-ultrasound/MY00777
- Mayo Clinic. "Preeclampsia." (Aug. 9, 2011) http://www.mayoclinic.com/health/preeclampsia/DS00583/DSECTION=complications
- Mayo Clinic. "Pregnancy week by week." (Aug. 9, 2011) http://www.mayoclinic.com/health/prenatal-testing/MY01403
- Mayo Clinic. "Rh factor blood test." (Aug. 9, 2011) http://www.mayoclinic.com/health/rh-factor/MY01163/DSECTION=why-its-done
- National Center for Biotechnology Information. "Gestational Diabetes." Sept. 11, 2010. (Aug. 9, 2011) http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0001898/
- National Center for Biotechnology Information. "Group B streptococcal septicemia of the newborn." Dec. 10, 2009. (Aug. 9, 2011) http://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0002342/
- Patient.co.uk. "Pre-eclampsia." (Aug. 9, 2011) http://www.patient.co.uk/health/Pregnancy-Pre-Eclampsia.htm
- pregnancy.org. "Urine Test During Pregnancy." (Aug. 9, 2011) http://www.pregnancy.org/article/urine-test-during-pregnancy-urinalysis



























